
The most recent state report on trauma care notes that there are five Level I adult trauma centers in Tennessee, two Level II centers, six Level III centers, and one provisional Level III center; but only 53% of injured Tennesseans are treated in Tennessee trauma centers. And according to a national study by the New England Journal of Medicine, the likelihood of survival increases by 25% when an injured adult receives treatment at a trauma center instead of a regular hospital. With the number of trauma victims increasing annually, the most patients being elderly suffering from a fall followed by automobile accident victims, a Level II trauma center in the county will mean saving more lives.
Once Saint Thomas Rutherford Hospital becomes a Level II trauma center in 2024, it will join Tri-Star Skyline Hospital in Nashville and Bristol Regional Medical Center as only the third in Tennessee. Vanderbilt University Medical Center is the only Level I trauma center in the area. This upgrade will ensure Rutherford County residents, and those who use the county as a regional medical facility, will have an increased level of emergency services and better traumatic outcomes.
Where Saint Thomas Rutherford has had to depend on transfer agreements to get the severely injured to hospitals with the capabilities to treat them, with the new designation and increased resources there will not only be less transfers to other hospitals, but smaller regional hospitals in Cannon, Bedford and other outlying counties will be able to have their severely injured sent to Saint Thomas Rutherford, instead of having to transport them all the way to Nashville. When someone is fighting for their life, the less time it takes to get to a treatment facility, the better the chance of survival.
While the American Trauma Society (ATS) defines the level of care for each designation, the level designations vary to some extent by state. In Tennessee, the state Trauma Advisory Council helps legislators define the regulations. A Level II Trauma Center, as defined by the ATC, “is able to initiate definitive care for all injured patients.” The elements of care at a Level II Trauma Center must include 24-hour immediate coverage by general surgeons, as well as coverage by specialties in orthopedic surgery, neurosurgery, anesthesiology, emergency medicine, radiology and critical care; provide trauma prevention and continuing education programs for staff; and [i]ncorporate a comprehensive quality assessment program. Other requirements include fully staffed operating rooms, lab and radiologic capabilities, and a specific number of dedicated intensive care beds.
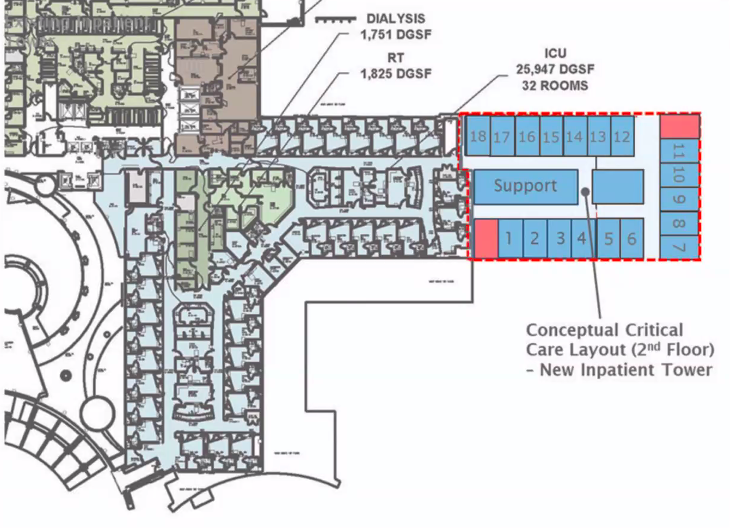 As part of their preparations, Saint Thomas Rutherford will improve their emergency department by building an additional 16 critical care unit beds on the second floor of the east tower, reconfigure the second floor to support expanded operating rooms, add eight emergency examination rooms, and also add additional CT and x-ray capacity, as well an onsite lab that will be able to do blood work in about 20 minutes. Additional staff will include four general surgeons, so one is on site 24/7 every day of the year.
As part of their preparations, Saint Thomas Rutherford will improve their emergency department by building an additional 16 critical care unit beds on the second floor of the east tower, reconfigure the second floor to support expanded operating rooms, add eight emergency examination rooms, and also add additional CT and x-ray capacity, as well an onsite lab that will be able to do blood work in about 20 minutes. Additional staff will include four general surgeons, so one is on site 24/7 every day of the year.
“Our open-heart surgery program, which will begin in 2023, will support the Level II Trauma Center,” said Gordon Ferguson, President and CEO of Saint Thomas Rutherford. “And we will be adding two more heart surgeons.”
The Trauma Team will be led by Dr. Eric Barquist, assisted by Dr. Habeeba Park. The I house emergency team will also include Dr. Tiffany Bee.
Designation as a Level II Trauma Center will be the culmination of many years of planning and building of both staff and physical plant, but when it occurs, it will put Saint Thomas Rutherford Hospital on the map as an even stronger regional medical facility.














